Complete Decongestive Therapy (CDT): The Gold Standard for Lymphedema Treatment
Lymphedema is a chronic condition caused by impaired lymphatic flow, often leading to swelling, discomfort, and an increased risk of infection. While there’s no cure, Complete Decongestive Therapy (CDT) remains the most effective, evidence-based treatment for reducing swelling and improving quality of life.
If you’re looking for ways to manage lymphedema after breast surgery or other procedures, understanding CDT is a critical first step.
What Is Complete Decongestive Therapy (CDT)?
Complete Decongestive Therapy (CDT) is a multi-component program designed to:
Improve lymphatic drainage
Reduce swelling in affected limbs
Maintain long-term function
CDT is typically delivered by certified lymphedema therapists, including physical therapy and occupational therapy specialists. The therapy is structured in two phases:
Intensive Phase – Frequent therapy sessions focused on rapid reduction of swelling
Maintenance Phase – Long-term strategies to maintain results and prevent recurrence
Tip: If you’re recovering from breast cancer surgery, consider combining CDT with a prehabilitation program to optimize your recovery.
Core Components of CDT
-
Manual Lymphatic Drainage is a gentle massage technique that stimulates the flow of lymph fluid. Key benefits include:
Reducing swelling and heaviness
Improving circulation
Decreasing discomfort
Therapists follow precise lymphatic pathways to maximize fluid movement safely. Learn more about manual lymph drainage techniques for post-surgical recovery.
-
MLD will not work unless you have the proper compression during the decongestion phase. This is what stops the fluid from coming back between sessions.
Here is why it works: when you move your muscles during everyday activity, the compression garments press back against your tissue. That pressure acts like a gentle squeeze, pushing fluid through the lymphatic vessels and preventing it from pooling again. Without this compression applied right after MLD, most of the progress made during the session reverses within a few hours.
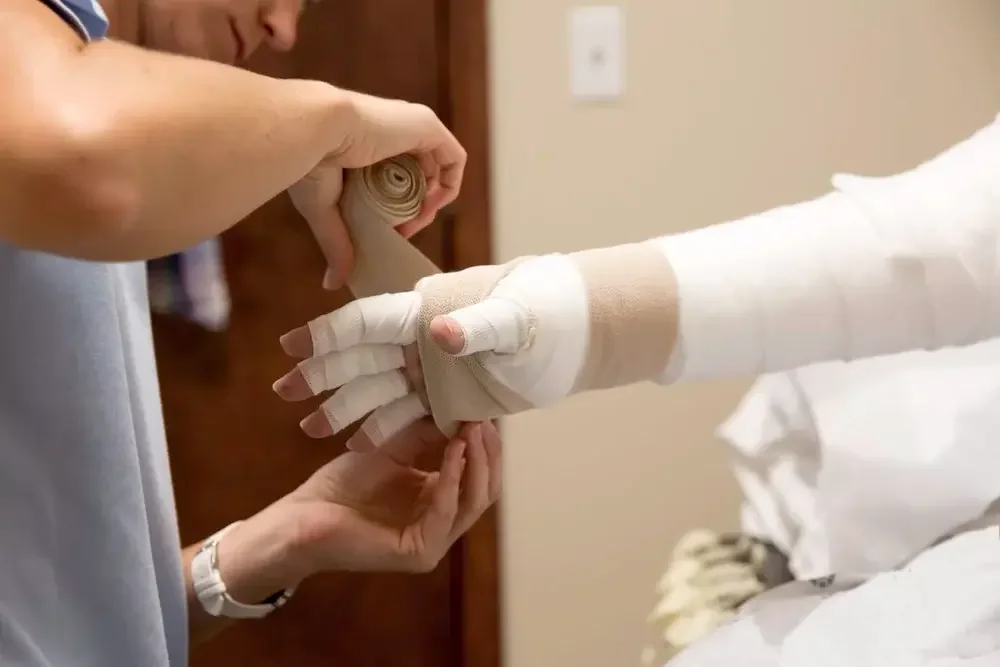
Compression is critical to maintain results from MLD. It may include:
Layered bandaging during the intensive phase
Custom compression garments (sleeves, gloves, or stockings) for maintenance
Proper fitting is essential. Check out our guide to post-surgical compression garments for tips on sizing and care.
-
Targeted exercises support lymph flow and maintain joint mobility. Benefits include:
Stimulating lymphatic circulation
Preserving shoulder and arm function
Strengthening surrounding muscles
Exercises are low-impact and tailored to your treatment stage. Consider pairing CDT with prehabilitation exercises before breast surgery to maximize recovery outcomes.
-
Lymphedema increases the risk of infections like cellulitis. CDT emphasizes:
Daily skin inspection
Moisturizing and protecting the skin
Promptly treating minor cuts
Proper skin care reduces complications and supports long-term lymphatic health. Learn more about skin care strategies for lymphedema.
Benefits of Complete Decongestive Therapy
Patients often experience:
Reduced swelling and limb volume
Improved comfort, mobility, and daily function
Lower risk of infection
Enhanced long-term control with self-care
CDT addresses all aspects of lymphedema, which is why it is widely considered the gold standard.
Why a CLT Certified Therapists Matter
Working with a therapist certified in lymphedema care (CLT) ensures:
Safe, effective manual lymphatic drainage
Proper compression garment application
Customized exercise programs
Ongoing monitoring and adjustments
For those recovering from breast surgery, combining CDT with lymphedema baseline measurements allows therapists to track progress and detect swelling early.
Maintenance and Long-Term Management
After the intensive phase, long-term management includes:
Consistent use of compression garments
Home-based self-massage or simplified MLD techniques
Regular monitoring for swelling or changes in limb volume
Lifestyle adjustments to support lymphatic health
Who Can Benefit from Complete Decongestive Therapy (CDT)?
Complete Decongestive Therapy (CDT) is the gold standard treatment for Lymphedema and is effective for anyone experiencing swelling or at risk for lymphatic complications. Understanding who can benefit from CDT helps patients and caregivers take proactive steps to prevent long-term swelling and improve mobility.
-
Patients who have had mastectomy, lumpectomy, or axillary lymph node removal are at higher risk for post-surgical swelling. CDT reduces swelling, helps prevent Lymphedema development and maintains shoulder and chest mobility.
-
Primary lymphedema: Congenital or hereditary lymphatic system issues
Secondary lymphedema: Resulting from surgery, radiation, trauma, or infection
CDT improves lymphatic flow, reduces swelling, and enhances overall function. Link “lymphedema management” to your main lymphedema treatment page.
-
Any procedure or injury affecting lymphatic pathways can cause temporary or chronic swelling. CDT helps restore fluid balance, discomfort and improve tissue mobility.
-
chronic swelling can lead to tissue hardening and limited mobility. CDT addresses soft tissue mobility, pain reduction, functional improvement, and swelling control.
-
Early CDT intervention can prevent severe swelling, reduce complications, and maintain limb health.
Why Early Intervention Matters
Starting CDT at the first signs of swelling or as a preventive measure can dramatically improve outcomes. Certified lymphedema therapists use baseline arm measurements, compression therapy, and guided exercises to monitor progress and customize treatment.
External backlink opportunity: Link authoritative sources such as the National Lymphedema Network for credibility.
Frequently Asked Questions:
-
The amount of time needed for Phase I will depend on the severity however a customized timeline will be laid out during the first session. Phase II is h periodic follow-up visits. Your therapist will give you a realistic timeline at your first appointment based on your specific situation.
-
No. The MLD portion uses very light pressure and should feel comfortable throughout. Compression bandaging can feel tight and slightly restrictive but it should not cause pain, numbness, or tingling. If it does, let your therapist know right away so they can adjust the wrap.
-
CDT is a structured clinical program that includes MLD, compression, exercise, skin care, and education, performed by a certified lymphedema therapist. A spa lymphatic massage does not include compression, is not performed by a certified therapist, and is not designed to treat lymphedema. For managing lymphedema, CDT is the standard of care.
-
No. New York State Direct Access allows you to start physical or occupational therapy without a doctor's referral for your first 10 visits or 30 days, whichever comes first. After that, a prescription from a physician is required. If you have a surgeon or oncologist involved in your care, your Thera therapist will communicate with them directly and send regular progress updates.
-
CDT can be adapted for patients who are currently receiving chemotherapy or radiation. Your specialized therapist will work with your oncology team to make sure the timing and approach are appropriate for where you are in treatment. Starting CDT during active treatment rather than waiting until after can prevent your lymphedema from progressing further.