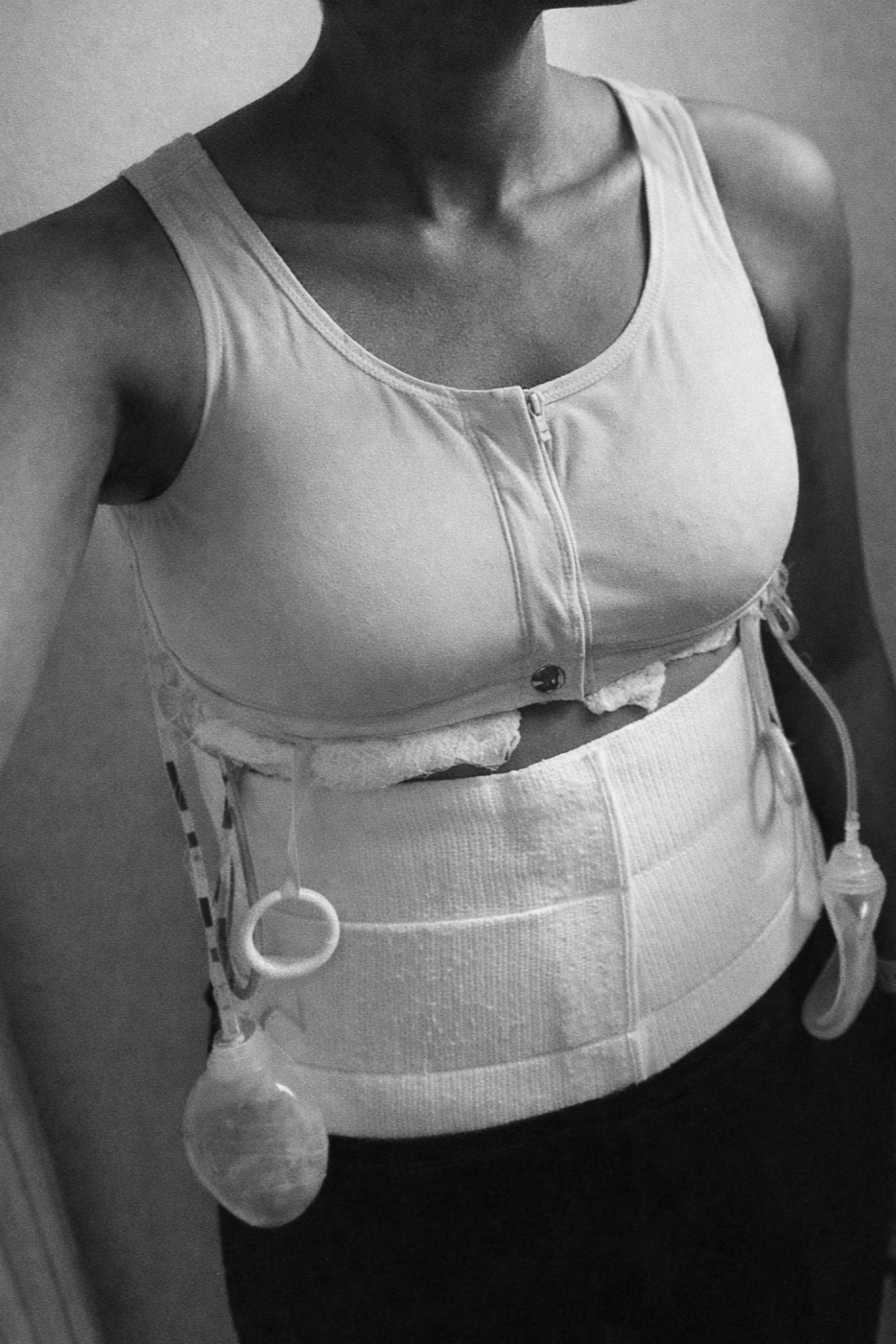
Breast Rehabilitation Should Be Standard After DIEP Flap Reconstruction
Recently, we had a patient in our clinic who told us her surgeon left it up to her whether she wanted physical or occupational therapy after her DIEP surgery. We still find it difficult to believe that, after everything a patient goes through with DIEP flap breast reconstruction, rehabilitation is still treated like an optional add-on.
Breast rehabilitation should be part of the standard of care, not something patients have to research, request, or fight for on their own.
The Reality of DIEP Flap Reconstruction Recovery
A DIEP flap reconstruction is one of the most advanced forms of breast reconstruction. It restores the breast using the patient’s own tissue, often following a mastectomy. But while the focus is rightly on surgical success, the recovery tells a much more complex story.
Patients are simultaneously healing from:
Major abdominal surgery
Chest wall trauma
Nerve disruption and altered sensation
Significant changes to posture and movement patterns
And yet, many patients are sent home with minimal guidance beyond basic precautions. That’s a gap that has real consequences.
Why Is Rehabilitation Still Treated as Optional?
In most areas of medicine, this wouldn’t happen. After a knee replacement, physical therapy is expected. After a stroke, rehabilitation is automatic. But after breast reconstruction, a procedure that impacts the chest, core, lymphatic system, and overall function, patients are often left to figure things out on their own.
That gap places an unfair burden on the individual. Patients shouldn’t have to ask:
“Do I need physical therapy or occupational therapy?”
“Is this abdominal tightness normal?”
“Why does my shoulder feel restricted?”
“I know I have to keep a flexed posture but when can I start extening after a DIEP surgery”
The system should already be answering those questions — with action.
What Breast Rehabilitation Actually Addresses After DIEP Flap Surgery
Breast rehab is not just about exercises. It’s about restoring function, reducing complications, minimizing scarring, and helping patients feel like themselves again. Our full breast cancer rehabilitation program is designed to address all of these areas systematically and safely.
Mobility and Functional Recovery
After DIEP flap surgery, it’s common to experience shoulder stiffness, abdominal pulling or tightness, limited range of motion, and difficulty standing fully upright. Without intervention, these patterns can persist for months or longer and compound into chronic dysfunction.
Scar Tissue and Internal Tightness
Scar tissue doesn’t just sit on the surface. It creates internal restrictions that affect movement and comfort at both the chest wall and the abdominal donor site. Our scar management and tissue therapy help improve tissue mobility, reduce tightness and pulling sensations, and prevent long-term fibrosis or scar adherence.
Pain and Postural Changes
Many patients unconsciously adapt their posture after surgery — rounding forward, guarding the chest, or avoiding certain movements. Over time, this leads to neck and back pain, muscle imbalances, and chronic discomfort that becomes increasingly difficult to unwind.
Lymphatic Health and Lymphedema Prevention
Patients undergoing breast reconstruction — particularly those who have had lymph nodes removed or radiated — benefit significantly from lymphatic care. Rehabilitation plays a key role in supporting lymphatic drainage, reducing swelling, and educating patients on early warning signs. Learn more about our lymphedema prevention and treatment program.
The Emotional Side of DIEP Flap Recovery
This part often gets overlooked. Recovery from breast reconstruction isn’t just physical, it’s deeply personal. Patients are navigating changes in their bodies, identities, and sense of normalcy.
Rehabilitation provides something more than physical treatment: reassurance, guidance, and a sense of measurable progress. It gives patients a place where their concerns are heard and addressed, not dismissed.
This Shouldn’t Be Left to the Patient to Figure Out
When rehabilitation is optional, access becomes inconsistent. Some patients receive comprehensive care. Others receive none simply because they didn’t know to ask. That’s not patient-centered care. That’s a gap in the system.
Breast rehabilitation after DIEP flap reconstruction should be:
Automatically included in every patient’s recovery plan
Introduced before surgery, when possible, not only after complications arise
Presented as essential care, not an elective add-on
A Better Standard of Care for Breast Reconstruction Patients
In New York City, more providers, including Thera, are working to change this by integrating rehabilitation into the recovery process from the very beginning. Our approach connects prehab, post-surgical care, and long-term survivorship support into a seamless continuum.
This approach leads to faster and more comfortable healing, fewer long-term complications, and better overall quality of life. Learn more about how our breast cancer rehabilitation program works, and explore how things work at Thera to take the first step.
The Bottom Line
Patients going through DIEP flap reconstruction have already made a major, courageous decision for their health and well-being. They shouldn’t have to navigate recovery alone, and they shouldn’t have to advocate for care that should already be on the table.
Rehabilitation is not something to “consider.” It is a necessary part of healing, and it should be treated that way.
Contact our team today to learn more or to schedule a consultation at our Midtown Manhattan clinic.
Frequently Asked Questions
-
Yes, it is highly beneficial and, in our clinical view, should be considered standard care. Rehabilitation restores mobility, reduces pain, prevents scar tissue complications, and supports lymphatic health in ways that rest alone cannot achieve.
-
Many patients can begin gentle rehabilitation around 3 weeks after surgery, depending on their surgeon’s recommendations and individual healing. Prehab, beginning care before surgery, is also an option and is associated with better post-surgical outcomes.
-
Unfortunately, no, which is exactly why advocacy for standardizing this care is so important. In New York State, patients can access physical and occupational therapy directly without a physician’s referral for up to 10 visits or one month, so you do not need to wait for a referral to begin.
-
Breast rehabilitation is a specialized area of care within our clinic. Regardless of discipline, both physical and occupational therapists who treat breast oncology patients complete the same advanced training, coursework, certifications, and rigorous mentorship under our senior staff.
Both physical and occupational therapy focus on restoring movement, strength, and function, as well as optimizing scar management. Our team includes highly trained specialists across both disciplines to ensure comprehensive, consistent care for every patient.